Pelvic Floor Therapy for Men
When we talk about “core strength,” most men envision chiseled abdominals or a powerful lower back. However, there is a literal “floor” to your core that remains largely ignored until it starts to fail. Imagine a sophisticated hammock of muscles stretching from your tailbone to your pubic bone, supporting your bladder and bowel while playing a lead role in sexual function. This is the pelvic floor—a powerhouse of stability that, when dysfunctional, can turn daily life into a series of uncomfortable or embarrassing hurdles.
For men navigating pelvic pain, urinary dysfunction, or post-operative recovery, the journey to finding specialized care can feel isolating. Fortunately, the landscape of rehabilitative medicine is shifting. Residents seeking Physiotherapy Hospitals in Bandlaguda are increasingly discovering that pelvic health isn’t just a “women’s issue.” At Rishitha Hospitals, we are bridging this gap, offering evidence-based Pelvic Floor Therapy (PFT) designed specifically for the male anatomy. Whether you are an athlete dealing with mysterious groin pain or a senior recovering from prostate surgery, understanding this muscular foundation is the first step toward reclaiming your quality of life.
The Hidden Engine: Understanding the Male Pelvic Anatomy
Before diving into therapy, we must dismantle the myth that men don’t have a pelvic floor worth mentioning. In the male body, these muscles wrap around the base of the penis and the rectum. They are responsible for three primary “S” functions: Support (keeping organs in place), Sphincter (controlling the flow of urine and stool), and Sexual (maintaining erections and climax).
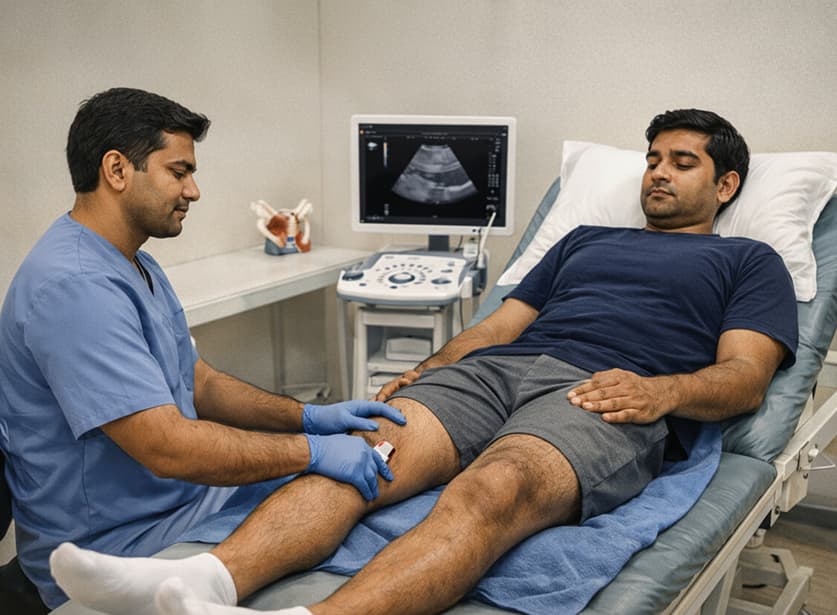
Shutterstock
When these muscles become too tight (hypertonic) or too weak (hypotonic), the system breaks down. Unlike a bicep strain that you can see and ice, pelvic floor dysfunction is internal and often manifests as referred pain. This is why specialised Physiotherapy Hospitals in Bandlaguda emphasie a clinical approach that looks beyond the symptoms to find the muscular root cause.
Beyond Kegels: The Unique Sub-Topics of Male Pelvic Rehab
1. The “Hard-Flaccid” and Chronic Pelvic Pain Syndrome (CPPS)
One of the most misunderstood conditions in male health is CPPS. Often misdiagnosed as recurring prostatitis (inflammation of the prostate), research suggests that up to 90% of chronic prostate-related pain is actually neuromuscular. Men may feel a “golf ball” sensation in the perineum or sharp pain in the pelvis. Pelvic floor therapy focuses on “down-training” these muscles—teaching them how to relax through manual release and diaphragmatic breathing, rather than just strengthening them.
2. The Post-Prostatectomy Pivot
For men undergoing surgery for prostate cancer, urinary incontinence is a common and distressing side effect. The prostate sits right at the neck of the bladder; once removed, the pelvic floor muscles must work overtime to take over the job of the internal sphincter. Targeted PFT at facilities like Rishitha Hospitals provides a roadmap for “pre-hab” (strengthening before surgery) and post-op recovery to dry up leaks faster and restore confidence.
3. The Athletic Pelvic Floor: Stability for the Powerlifter and Cyclist
High-impact sports and heavy lifting put immense intra-abdominal pressure on the pelvic floor. If you aren’t breathing correctly during a squat, that pressure has nowhere to go but down. Conversely, cyclists often suffer from “pudendal neuralgia”—compression of the nerve that runs through the pelvic floor—leading to numbness or “cyclist’s syndrome.” Therapy involves biomechanical adjustments and pressure management to ensure your fitness routine doesn’t come at the cost of your pelvic health.
4. The Bowel Connection: Solving Chronic Constipation
Pelvic floor therapy is an effective, non-pharmacological treatment for dyssynergic defecation—a fancy term for when your muscles tighten instead of relaxing during a bowel movement. A pelvic therapist uses biofeedback to help men re-coordinate these muscles, ending the cycle of straining that leads to haemorrhoids and further muscle trauma.
What Happens During a Male Pelvic Therapy Session?
It is natural to feel a bit apprehensive about your first visit. However, the process is highly professional and clinical.
- Initial Assessment: Your therapist will discuss your urinary, bowel, and sexual history. They will analyse your posture, hip mobility, and breathing patterns.
- External and Internal Evaluation: A therapist may palpate the external muscles of the abdomen and thighs. If necessary, an internal assessment (via the rectum) is performed to directly check the tone and strength of the pelvic floor muscles.
- Biofeedback Technology: Using sensors, you can see your muscle activity on a screen in real-time. This helps you “find” muscles that you didn’t know you could control.
- Manual Therapy: This includes trigger point release and myofascial stretching to alleviate “knots” within the pelvic bowl.
The Neurological Link: Stress and the Pelvic Floor
The pelvic floor is often referred to as the “emotional barometer” of the body. Just as some people clench their jaw or shrug their shoulders when stressed, many men subconsciously “tuck” their tailbone and tighten their pelvic floor. Over the years, this chronic tension leads to pain and urinary frequency. Pelvic floor therapy integrates nervous system regulation, teaching men how to shift from a “fight or flight” state to a “rest and digest” state, which is essential for muscle relaxation.
Frequently Asked Questions (FAQs)
- Is pelvic floor therapy only for men who have had surgery?
No. While it is crucial for post-prostatectomy recovery, PFT is highly effective for chronic pelvic pain, erectile dysfunction, “prostatitis-like” symptoms, and chronic constipation. Anyone experiencing pelvic discomfort or urinary urgency can benefit from an evaluation.
- How long does it take to see results from male pelvic floor therapy?
Most patients begin to notice significant changes within 4 to 8 weeks of consistent therapy. However, because every condition—from nerve entrapment to muscle weakness—is unique, your therapist will provide a personalised timeline during your initial assessment.
- Does pelvic floor therapy help with erectile dysfunction (ED)?
Yes, in many cases. If ED is caused by poor blood flow or weak pelvic muscles (which help trap blood in the penis), PFT can improve the strength and duration of erections. It is often used as a complementary treatment alongside medical interventions.
- What should I wear to my physiotherapy appointment?
Wear comfortable, loose-fitting clothing, similar to what you would wear for a standard physical therapy session or a gym workout. This allows your therapist to easily assess your hips, spine, and abdominal movement.
- Can I do these exercises at home on my own?
While “home programs” are a vital part of recovery, it is dangerous to guess. Doing Kegels when your muscles are already too tight (hypertonic) can actually worsen your pain. An initial professional evaluation is essential to determine if you need to strengthen or relax your muscles.
Pelvic floor therapy is not a sign of weakness; it is a sophisticated tool for physical optimisation. No man should have to “just live” with pain or leakage. By seeking expert guidance at specialised centres, you are investing in your long-term mobility and intimate health. At Rishitha Hospital, we prioritise your privacy and progress, ensuring that every man has the support needed to build a stronger, more resilient foundation from the inside out.