Overview of PCOD and PCOS
Polycystic Ovarian Disease (PCOD) and Polycystic Ovarian Syndrome (PCOS) are frequently confused, yet distinct hormonal conditions affecting the reproductive system. While PCOD is characterized by the release of immature eggs due to hormonal imbalances, PCOS is recognized as a more severe metabolic disorder. Effective management is essential for long-term health and reproductive success. For those seeking specialized guidance, expert care is provided by Fertility Hospitals in Bandlaguda, including Rishitha Hospitals. Early diagnosis through medical consultation ensures that symptoms are controlled and fertility potential is preserved through personalized lifestyle interventions and clinical treatments tailored to individual hormonal profiles.
PCOD vs. PCOS: A Comprehensive Guide to Hormonal Health
Hormonal health is often considered the cornerstone of overall well-being for women. Among the various endocrine challenges encountered during the reproductive years, PCOD (Polycystic Ovarian Disease) and PCOS (Polycystic Ovarian Syndrome) are the most prevalent. Although these terms are often used interchangeably in casual conversation, significant physiological and clinical differences are identified by medical professionals. Understanding these nuances is vital for effective symptom management and the prevention of long-term complications.
Defining the Conditions
PCOD is regarded as a condition where the ovaries produce immature or partially mature eggs in large numbers. These follicles eventually turn into cysts. It is generally attributed to a combination of lifestyle factors, stress, and minor hormonal fluctuations. Conversely, PCOS is classified as a metabolic disorder involving a more profound imbalance of the endocrine system. In PCOS, higher levels of androgens (male hormones) are produced by the ovaries, which interferes with the regular ovulation process.
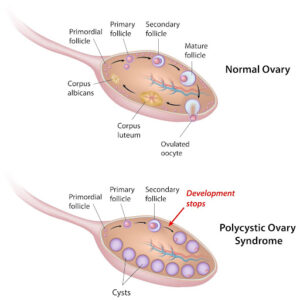
The Pathophysiology of PCOD and PCOS
The mechanisms behind these conditions are complex. In the case of PCOD, the normal cycle of egg maturation is disrupted. Usually, one egg is released every month, but when the hormonal environment is slightly altered, multiple eggs remain in the ovaries in an underdeveloped state.
In PCOS, the endocrine disruption is more systemic. High levels of insulin resistance are frequently observed in patients. When the body becomes resistant to insulin, more of this hormone is produced by the pancreas to compensate. Consequently, the ovaries are stimulated to produce excessive amounts of testosterone. This hormonal cascade leads to the characteristic symptoms of the syndrome, such as irregular periods, hirsutism, and acne.
Comparative Symptoms and Identification
While an overlap in symptoms is noted, the intensity and range differ between the two.
- Menstrual Irregularities: Infrequent or prolonged periods are experienced by individuals with both conditions. However, in PCOS, menstruation may be completely absent for several months.
- Physical Changes: Weight gain, particularly around the abdominal area, is commonly reported. Excessive hair growth on the face and body (hirsutism) and thinning of hair on the scalp are frequently observed in PCOS cases due to androgen dominance.
- Skin Health: Persistent acne and darkening of the skin (acanthosis nigricans) are considered clinical markers of insulin resistance often associated with PCOS.
- Fertility Impacts: While PCOD does not strictly prevent pregnancy, conception may be delayed. In contrast, PCOS is identified as a leading cause of female infertility because ovulation is significantly impaired.
Diagnostic Procedures
A diagnosis is typically reached through a multi-faceted approach. Clinical history is thoroughly reviewed by specialists to track menstrual patterns. Physical examinations are conducted to identify signs of androgen excess.
Furthermore, blood tests are utilized to measure hormone levels, including LH (Luteinizing Hormone), FSH (Follicle-Stimulating Hormone), and testosterone. Ultrasound imaging is employed to visualize the ovaries; a “string of pearls” appearance is often detected when multiple follicles are present. Metabolic screening, including glucose tolerance tests, is also recommended to assess insulin sensitivity.
Management and Treatment Strategies
Although these conditions cannot be completely “cured” in the traditional sense, they are effectively managed through various interventions.
Lifestyle Modifications
The foundation of management is built upon lifestyle changes. A balanced diet low in refined sugars and high in fiber is recommended to stabilize insulin levels. Regular physical activity is encouraged to improve metabolic rate and aid in weight management. Even a modest reduction in body weight is shown to restore regular ovulation in many instances.
Pharmacological Interventions
When lifestyle changes are insufficient, medication is prescribed. Hormonal contraceptives are frequently used to regulate the menstrual cycle and reduce androgen levels. For those struggling with insulin resistance, metformin may be administered. If pregnancy is desired, ovulation-inducing medications are utilized under strict medical supervision.
Holistic Approaches
Stress management techniques, such as yoga and meditation, are found to be beneficial in balancing cortisol levels, which in turn supports reproductive health. Adequate sleep and the avoidance of endocrine disruptors found in certain plastics and chemicals are also advised.
Long-Term Health Implications
If left unmanaged, PCOS can lead to serious health complications later in life. A higher risk of Type 2 diabetes, cardiovascular disease, and hypertension is associated with the metabolic disturbances of the syndrome. Additionally, prolonged absence of menstruation can lead to an increased risk of endometrial hyperplasia. Therefore, regular monitoring by healthcare providers is essential.
Seeking Specialized Care
For residents in the Hyderabad region, access to high-quality diagnostic and treatment facilities is available. Comprehensive evaluations and advanced treatment protocols are offered by specialized centers. Expert guidance is provided by professionals at leading institutions to ensure that every patient receives a tailored management plan.
Frequently Asked Questions (FAQs)
- Is it possible to get pregnant with PCOD or PCOS?
Yes, pregnancy is achievable with both conditions. While PCOD may only require minor lifestyle adjustments to regulate ovulation, PCOS often necessitates specialized medical intervention and fertility treatments to facilitate conception.
- What is the primary difference between PCOD and PCOS?
PCOD is considered a common condition where ovaries release immature eggs due to lifestyle factors, whereas PCOS is a more severe metabolic disorder characterized by high androgen levels and systemic hormonal imbalances.
- Can PCOS be managed without medication?
In some mild cases, symptoms are successfully managed through significant lifestyle changes, including a strict diet and regular exercise. However, medication is often required for more severe hormonal disruptions or when fertility is a primary concern.
- Does PCOD lead to permanent infertility?
No, PCOD does not cause permanent infertility. With proper management of diet, stress, and weight, regular ovulation is usually restored, allowing for natural conception.
- Why is weight gain so common in these conditions?
Weight gain is primarily driven by insulin resistance, which is frequently associated with PCOS. This metabolic state causes the body to store fat more easily and makes weight loss more challenging compared to those with balanced hormones.
Navigating the complexities of PCOD and PCOS can feel overwhelming, but understanding the distinction is the first step toward reclaiming your hormonal health. Whether you are managing mild symptoms or addressing metabolic challenges, proactive care is key to preventing long-term complications and ensuring reproductive success.
Prioritize your well-being today. For personalized treatment plans and expert guidance, consult Rishitha Hospitals, where specialized care meets compassionate support.