Overview of Laparoscopic and Open Surgery
Modern surgical techniques have shifted significantly toward patient-centric recovery, making the debate between laparoscopic and open surgery more relevant than ever. While traditional open surgery involves larger incisions, laparoscopic methods utilize minute openings and advanced imaging to perform complex procedures with precision. This minimally invasive approach is increasingly recognized as the future of surgery due to its ability to reduce physical trauma and hospital stays. For those seeking advanced care, finding the best hospital in Bandlaguda is essential. Rishitha Hospitals stands as a leader in this field, offering cutting-edge surgical solutions that prioritize safety and faster healing.
The Evolution of Surgery: Why Minimally Invasive Procedures are Redefining Healthcare
For decades, the standard approach to internal medical issues was open surgery. Large incisions were required so that surgeons could directly visualize and access organs. However, the landscape of medical science has been transformed by the advent of laparoscopic techniques. Often referred to as “keyhole surgery,” laparoscopy is no longer just an alternative; it is being established as the gold standard for a wide variety of abdominal and pelvic procedures.
Understanding the Fundamental Differences
The primary distinction between these two methods lies in the access point. In open surgery, a single, large incision is made through the skin and muscle layers. This allows the surgeon a full view of the surgical field. While effective, the extensive nature of the wound often leads to significant postoperative pain and a lengthy recovery period.
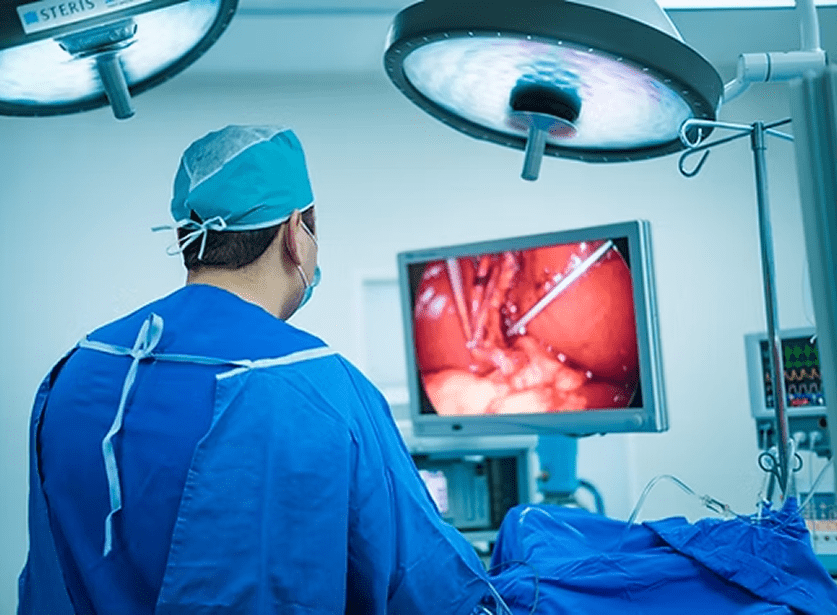
In contrast, laparoscopy is performed through several small incisions, usually no larger than 0.5 to 1.5 centimeters. A specialized camera called a laparoscope is inserted into one of these openings. High-definition images are then transmitted to a monitor in the operating room, providing a magnified view of the internal structures. Specialized, slender instruments are manipulated through the other small ports to perform the necessary repairs or removals.
The Clinical Advantages of the Minimally Invasive Approach
The shift toward minimally invasive surgery is driven by several clinical benefits that directly impact patient outcomes.
- Reduced Blood Loss: During laparoscopic procedures, the precision offered by magnified imaging allows for better control of blood vessels. Consequently, the need for blood transfusions is significantly minimized compared to open operations.
- Lower Risk of Infection: Because the internal organs are not exposed to the external environment for prolonged periods, the risk of airborne contamination is greatly reduced. Smaller wounds also mean there is less surface area susceptible to localized infections.
- Diminished Postoperative Pain: Since large muscle groups are not severed, the inflammatory response of the body is less intense. This results in a decreased reliance on heavy pain medications and opioids during the recovery phase.
- Minimal Scarring: From an aesthetic and physiological standpoint, small puncture marks heal far more cleanly than long, linear scars. The risk of developing incisional hernias later in life is also notably lower with laparoscopy.
Faster Recovery and Return to Normalcy
One of the most compelling reasons why laparoscopy is viewed as the future of surgery is the speed of recovery. In the traditional open approach, patients are often required to remain hospitalized for a week or more to monitor wound healing and bowel function. With the minimally invasive route, many procedures are now performed on an outpatient basis, or require only an overnight stay.
Normal activities, such as walking, driving, and returning to work, are typically resumed within days rather than months. This efficiency not only benefits the patient’s quality of life but also reduces the economic burden of long-term healthcare costs and lost productivity.
Enhanced Precision through Technology
The “future” of this field is also being shaped by robotic-assisted laparoscopy. In these cases, the instruments are controlled by a surgeon via a computer console. This provides an even greater range of motion—exceeding that of the human wrist—and eliminates the tiny tremors that can occur during manual surgery. Complex oncological resections and intricate reconstructive surgeries are being performed with a level of accuracy that was previously thought to be impossible.
Addressing the Limitations
It must be noted that while laparoscopy is preferred, it is not always feasible. In cases of extreme obesity, severe internal scarring from previous surgeries, or complex emergency traumas, the open approach may still be deemed the safest option by a surgical team. The decision is always guided by the goal of ensuring the best possible survival and health outcomes for the individual.
Frequently Asked Questions (FAQs)
- Is general anesthesia required for laparoscopic surgery?
Yes, general anesthesia is typically administered for laparoscopic procedures. This is done to ensure that the patient remains completely still and pain-free, and to allow the abdominal muscles to be fully relaxed while the abdomen is inflated with carbon dioxide for better visibility.
- How long does the recovery process take after a minimally invasive procedure?
While every patient is different, most individuals are able to return to light activities within one to two weeks. This is significantly shorter than the six to eight weeks often required for recovery following a major open surgery.
- Are there any specific risks associated with laparoscopy?
Although it is considered very safe, risks can include minor complications from the carbon dioxide gas used during the procedure, such as temporary bloating or shoulder pain. Rare risks involving injury to adjacent organs or blood vessels are minimized by the use of high-definition cameras.
- Can all surgeries be performed laparoscopically?
Not all surgeries are candidates for a minimally invasive approach. The suitability of the technique is determined by the surgeon based on the patient’s medical history, the complexity of the condition, and the urgency of the operation.
- Will there be any visible scars after the surgery?
The scars resulting from laparoscopy are usually very small and fade significantly over time. Most incisions are so tiny that they eventually become barely noticeable, unlike the prominent scarring associated with traditional open surgery.
The transition toward minimally invasive surgery represents more than just a technological upgrade; it is a commitment to a better patient experience. By prioritizing smaller incisions, reduced pain, and faster returns to daily life, laparoscopic surgery has set a new benchmark for excellence in healthcare.
At Rishitha Hospitals, we believe that every patient deserves access to the most advanced surgical techniques in a supportive and safe environment. Our team of expert surgeons utilizes state-of-the-art technology to ensure that your path to recovery is as smooth and efficient as possible. Whether you are facing a routine procedure or a complex surgical challenge, you don’t have to settle for traditional methods when a modern, minimally invasive option is available.
Your health is your most valuable asset—trust it to the leaders in surgical innovation.